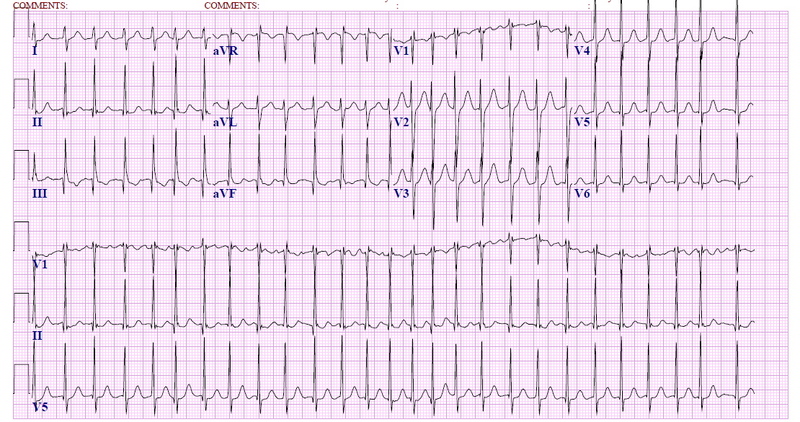
In this chapter, we will discuss the classification, pathophysiology, clinical presentation, electrocardiographic characteristics, electrophysiological testing and both the pharmacological and ablative management of atrial flutter. Re-entry however is still thought to play a role in atrial fibrillation, but its exact involvement is unknown. Currently these waves are considered chaotic and do not behave like the macro-reentry wavefront of atrial flutter. 
These mechanisms are distinct from that of atrial flutter which is macro-reentrant however, atrial tachycardia can also be re-entrant in mechanism similar to atrial flutter but on a microscopic level (re-entry around barriers of less than 2 cm).Ītrial fibrillation is due to fibrillatory waves in the atria with rates that are typically greater than 300 bpm in the atria. Its mechanism can be due to triggered activity or increased automaticity of atrial cells. As such, atrial flutter and atrial fibrillation often coexist.Ītrial tachycardia is typically characterised by atrial rates >100 bpm but less than 240 bpm with discrete activation sequences and non-sinus P waves including a baseline isoelectric period between these waves on ECG. If the tachycardia persists for a prolonged period, it frequently can degenerate into atrial fibrillation, particularly if the patient already has structural heart disease. It is generally paroxysmal in nature in a structurally healthy heart. The atrial rate in atrial flutter is approximately 240–360 beats per minute (bpm) with no distinct isoelectric period between the flutter ‘F’ waves. Atrial flutter has been traditionally defined as a macro-reentrant arrhythmia around a macroscopic (more than 2 cm in area) anatomical barrier that is confined within the atria. Although they are supraventricular in origin, apart from atrial tachycardia, they are not generally included in the nomenclature of supraventricular tachycardia. The more frequent clinically encountered atrial tachyarrhythmias include atrial tachycardia, atrial flutter and atrial fibrillation. Atrial arrhythmias are significant contributors for cardiac co-morbidity especially for stroke, heart failure and recurrent hospitalisations.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
